Measles
There has been a recent rise in measles cases in the UK. Although most children with measles can be looked after at home and do not require admission to hospital, a proportion develop severe complications including pneumonia (infection of the lungs) and encephalitis (swelling of the brain).
The most effective thing that you can do to protect your child against measles is to make sure that they receive 2 doses of the MMR vaccine (the 1st at 1 year of age, the 2nd at 3 years 4 months of age) – this will almost completely protect them from getting measles. Even if you or your children have missed these vaccines, it’s not too late to have them; contact your GP practice today. We have more information about the MMR vaccine on our website.
The initial symptoms of measles are:
a combination of fever, red eyes (conjunctivitis), runny nose, and cough. Your child may also develop some white spots inside their mouth and on the back of their lips:
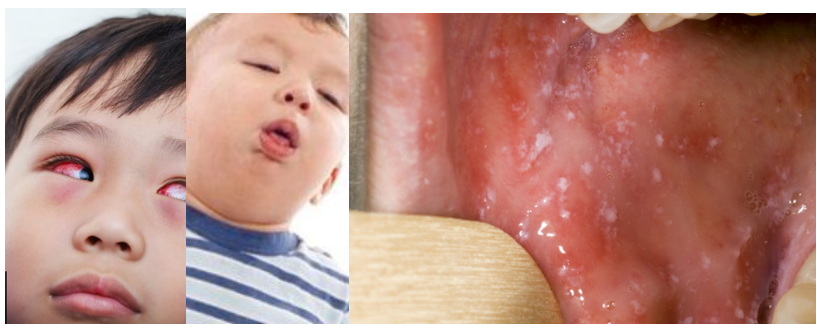
This is followed by a rash that appears a few days later – the rash usually begins behind the ears before spreading to the rest of the body. The spots of the measles rash are sometimes raised and often join together to form blotchy patches. They are not usually itchy.
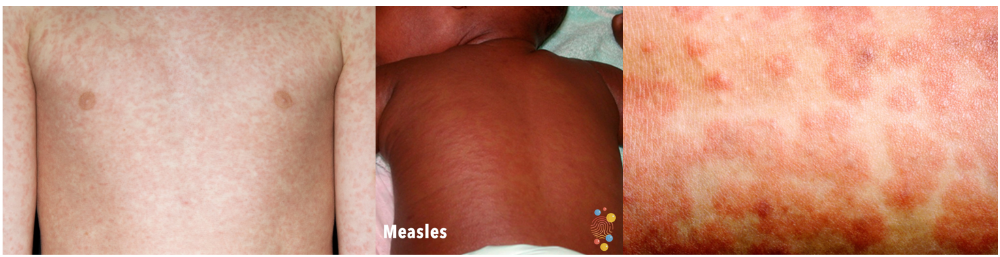
If your child has measles, they are likely to be unwell enough to need to spend a few days in bed and it may take about two weeks to be well enough to go back to school / nursery. Measles is easily spread from person to person (highly contagious); your child cannot go back to school/nursery until at least 4 days after the onset of the rash and should also avoid contact with pregnant women (who have not had 2 doses of the MMR vaccine) and people with weakened immune systems during this period.
If your child has had both doses of their MMR vaccine, there is almost no chance of them getting measles (unless they have a severely weakened immune system).
Even in developed countries such as the UK, around one in every 15 children with measles will develop more serious complications. These can include:
- ear infection (otitis media) in about 1 in 12 children with measles
- pneumonia (chest infection) in about 1 in 16 children with measles
- diarrhoea in about 1 in 12 children with measles
- encephalitis (inflammation of the brain): 1 case for every 1000-2000 children with measles. Encephalitis can lead to permanent brain damage
- measles causes death in about 1 in 5000 children with measles
Is measles serious?
Measles can be unpleasant, but will usually pass in about 7 to 10 days without causing any further problems.
Once you’ve had measles, your body builds up resistance (immunity) to the virus. It’s highly unlikely you’ll get it again. However, it is highly advisable to get vaccinated to reduce your chances of getting measles.
Measles can lead to serious and potentially life-threatening complications in some people. These include infections of the lungs (pneumonia) and brain (encephalitis).
If your child has any of the following features:
- Has blue lips
- Too breathless to talk / eat or drink
- Is pale, mottled and feels abnormally cold to touch
- Is extremely agitated (crying inconsolably despite distraction),
- Is confused or very lethargic (difficult to wake)
- Has a fit / seizure
- Has double vision or blurred vision
- Has a rash that does not disappear with pressure (the ‘Glass Test’)
You need urgent help.
Go to the nearest Hospital Emergency (A&E) Department or phone 999.
Measles can spread to others easily. Tell services before you go in. Let them know as soon as you arrive if your child has not been vaccinated against measles (MMR vaccine).
If your child has any of the following features:
- Has laboured/rapid breathing or they are working hard to breathe – drawing in of the muscles below their lower ribs, at their neck or between their ribs (recession).
- A harsh breath noise as they breathe in (stridor) present only when they are upset.
- Seems dehydrated (sunken eyes, drowsy or passed no urine for 12 hours)
- Is drowsy (excessively sleepy) or irritable (unable to settle them with toys, TV, food or picking up) – especially if they remain drowsy or irritable despite their fever coming down
- Has pus coming out of their ear
- Is 3-6 months of age with a temperature of 39°C / 102.2°F or above (but fever is common in babies up to 2 days after they receive vaccinations)
- Continues to have a fever of 38.0°C or above for more than 5 days
You need to contact a doctor or nurse today.
Please ring your GP surgery or call NHS 111 - dial 111
If your child has amber features and you are worried that they may have measles, contact your GP surgery or NHS 111 and let them know that your child might have measles. It is important that you let them know if your child has not been vaccinated against measles (MMR vaccine). Try to avoid turning up at your GP surgery unannounced as your child could spread the infection to others.
If symptoms persist for 4 hours or more and you have not been able to speak to either a member of staff from your GP practice or to NHS 111 staff, recheck that your child has not developed any red features.
- If none of the above features are present, most children with measles can be safely managed at home.
- However, if your child has measles, you still need to tell your GP practice as there may be other people that your child has come into contact with that may be at increased risk of severe infection.
Self care
Continue providing your child’s care at home. If you are still concerned about your child, speak to your health visitor, local pharmacist or call NHS 111– dial 111
Your child cannot go back to school or nursery until at least 4 days after the onset of their rash. This is to avoid them spreading measles to others.
What should you do?
-
Keep watching your child for signs of red and amber features (as mentioned above). If they develop, it might mean they have a more serious illness that needs specific tests and treatment. Ask for help in such cases.
-
To help your child feel better you can use paracetamol (calpol) and/or ibuprofen to lower their temperature. Try one medicine first, and if your child doesn't get better within 2-3 hours, you can try the other one. Remember, though, that fever is the body's normal response to fight infections, and the medicines won't make it go away completely.
-
Don't use tepid sponging on your child because it doesn't actually reduce their temperature and might make them shiver.
-
Encourage your child to drink lots of fluids.
-
If there are any crusts your child's eyes, gently remove them using cotton wool soaked in warm water.
- If you think your child has measles, let your GP practice and any healthcare setting know before you visit them. They might prefer to see you on video. Your child can spread the infection to others from the time their symptoms start until about four days after the rash appears.
- If you are pregnant and haven't received 2 doses of the MMR vaccine, or if there are any children in your family who are under 12 months old or haven't had 2 doses of the MMR vaccine, please inform your GP practice urgently, as they might need immediate treatment to protect them from getting measles. Make sure that you/your partner are up to date with your MMR vaccines before getting pregnant as measles can be extremely severe during pregancy and can harm your unborn baby.
- If your child with measles has been in contact with someone who has a very weak immune system (from the onset of their symptoms until four days after their rash begins), let that person know about your child's measles and ask them to contact their GP practice or NHS 111 urgently.
Where should you seek help?
- Unless your child has red features (see above), try to stay away from public places including pharmacists, GP practices and A&E departments as your child may spread their infection to others.
- If your child has any of the above amber features (see above), urgently contact your GP or call NHS 111. Make sure you let them know if your child has not been vaccinated against measles (MMR vaccine).
- You should only call 999 or go your nearest A&E department in critical or life threatening situations. Let a member of staff know as soon as you arrive if your child has not been vaccinated against measles (MMR vaccine).
For wear and tear, minor trips and everything in between.
Self-care
You can treat your child's very minor illnesses and injuries at home.
Some illnesses can be treated in your own home with support and advice from the services listed when required, using the recommended medicines and getting plenty of rest.
Sound advice
Children can recover from illness quickly but also can become more poorly quickly; it is important to seek further advice if a child's condition gets worse.
For information on common childhood illnesses go to What is wrong with my child?
Pharmacists are experts in many aspects of healthcare and can offer advice on a wide range of long-term conditions and common illnesses such as coughs, colds and stomach upsets. You don’t need an appointment and many have private consultation areas, so they are a good first port of call. Your pharmacist will say if you need further medical attention.
Sound advice
- Visit a pharmacy if your child is ill, but does not need to see a GP.
- Remember that if your child's condition gets worse, you should seek further medical advice immediately.
- Help your child to understand - watch this video with them about going to the pharmacy.
For information on common childhood illnesses go to What is wrong with my child?
Health visitors are nurses or midwives who are passionate about promoting healthy lifestyles and preventing illness through the delivery of the Healthy Child Programme. They work with you through your pregnancy up until your child is ready to start school.
Health Visitors can also make referrals for you to other health professionals for example hearing or vision concerns or to the Community Paediatricians or to the child and adolescent mental health services.
Contact them by phoning your Health Visitor Team or local Children’s Centre.
Sound advice
Health visitors also provide advice, support and guidance in caring for your child, including:
- Breastfeeding, weaning and healthy eating
- Exercise, hygiene and safety
- Your child’s growth and development
- Emotional health and wellbeing, including postnatal depression
- Safety in the home
- Stopping smoking
- Contraception and sexual health
- Sleep and behaviour management (including temper tantrums!)
- Toilet training
- Minor illnesses
For more information watch the video: What does a health visitor do?
School nurses care for children and young people, aged 5-19, and their families, to ensure their health needs are supported within their school and community. They work closely with education staff and other agencies to support parents, carers and the children and young people, with physical and/or emotional health needs.
Contacting the School Nurse
Primary and secondary schools have an allocated school nurse – telephone your child’s school to ask for the contact details of your named school nurse.
There is also a specialist nurse who works with families who choose to educate their children at home.
Sound Advice
Before your child starts school your health visitor will meet with the school nursing team to transfer their care to the school nursing service. The school nursing team consists of a school nursing lead, specialist public health practitioners and school health staff nurses.
They all have a role in preventing disease and promoting health and wellbeing, by:-
- encouraging healthier lifestyles
- offering immunisations
- giving information, advice and support to children, young people and their families
- supporting children with complex health needs
Each member of the team has links with many other professionals who also work with children including community paediatricians, child and adolescent mental health teams, health visitors and speech and language therapists. The school health nursing service also forms part of the multi-agency services for children, young people and families where there are child protection or safeguarding issues.
GPs assess, treat and manage a whole range of health problems. They also provide health education, give vaccinations and carry out simple surgical procedures. Your GP will arrange a referral to a hospital specialist should you need it.
Sound advice
You have a choice of service:
- Doctors/GPs can treat many illnesses that do not warrant a visit to A&E.
- Help your child to understand – watch this video with them about visiting the GP or going to a walk in centre
For information on common childhood illnesses go to What is wrong with my child?
If you’re not sure which NHS service you need, call 111. An adviser will ask you questions to assess your symptoms and then give you the advice you need, or direct you straightaway to the best service for you in your area.
Sound advice
Use NHS 111 if you are unsure what to do next, have any questions about a condition or treatment or require information about local health services.
For information on common childhood illnesses go to What is wrong with my child?
A&E departments provide vital care for life-threatening emergencies, such as loss of consciousness, suspected heart attacks, breathing difficulties, or severe bleeding that cannot be stopped. If you’re not sure it’s an emergency, call 111 for advice.


